Healthcare Analytics
We bring the necessary analytics capabilities that enable system-wide quality improvement and cost reduction efforts promising the ability to transform healthcare into a truly data-driven, value-based industry.

Financial risk is quickly shifting in the healthcare industry from the Payer to the Provider. Given this shift in risk to Providers, hospitals are becoming a data driven sector now more than ever before. The ACA has demanded improved outcomes with CMS incentivizing these performance metrics in this new value-based healthcare care continuum; creating a mantra of “follow your data to make the optimal decisions for the best patient and financial outcomes.”
iCube brings the necessary data analytics capabilities that enable system-wide quality improvements and cost reduction efforts that are needed to transform healthcare into a truly data-driven, value-based industry sector.
Did you know?
- By the end of 2016 50% of all hospitals will be using some sort of an advanced data analytics platform to run their operations.
- Healthcare as an industry widely lags in the use of data analytics as compared to many other sectors such as banking and retail mainly due to systemic issues around patient privacy which can easily be navigated around from a compliance perspective
- After 20 consecutive years of increasing costs, healthcare now represents 17.6% of the USA’s GDP
- When this same ratio is compared to other countries of similar size and wealth the USA is spending $600 billion more than expected with no real value to show for it (lowest life expectancy among similar countries)
- Gartner predicts by the year 2020 there will be more than 25 billion connected devices with healthcare oriented wearables driving most of that growth (i.e. internet of things)
- Since 2010 more than 200 new businesses have developed innovative healthcare apps with approx. 40% of these tools focused on predictive capabilities
- By 2018 CMS plans to move 50% of their payments away from FFS and migrate those claims into alternate value-based payment models

Big Data/Predictive Outcomes:
Healthcare as an industry is perfectly suited for big data analytics given the vast amount of data generated from the various disparate healthcare providers. It is estimated that up to 80% of the healthcare data sources are unstructured data containing non-uniform data types from this disconnected ecosystem and that is exactly what big data solves for. And making sense of these various data types/sources and identifying patterns and insights is where predictive analytics comes into play with big data. As an industry healthcare’s big data universe is where many of the healthcare cost savings are hidden. Cracking this hidden code represents a huge ROI potential to the healthcare industry.
Our Predictive Healthcare Analytics Readiness Assessment will help you:
- Gain a solid view of the current state of your expected organization touchpoints.
- Understand what potential gaps exist in your current human resources, infrastructure and IT capabilities
- Identify organizational systemic roadblocks that could impede a successful program being deployed
- Determine a strategic roadmap with priority stage gates for implementing a full solution in this space as it considered a best practice to do deploy this type of solution in stages
- Understand how to build a strong governance program/team to assure alignment throughout the organization with a focus on change management techniques
The assessment will take place over the course of a few weeks with key stakeholder interviews conducted as suggested by the Executive Sponsor and will also include observations and analysis of the current state of the organization’s processes, people, and policies. Check point status meetings will be held and final deliverable will be an in-person executive presentation.

Population Health
Another looming outcome from the ACA is an emerging area of healthcare called Population Health (PH). Commonly defined as managing health outcomes for entire population groups by using an integrated end to end approach throughout the entire healthcare care continuum (prevention thru cure). Longer term PH will encourage healthcare providers to move into an IDN care model to facilitate and enable this initiative to be truly successful.
The four main components of a sound PH program are:
- Multiple data types/sources
- Healthcare Analytics
- Integrated Care Coordination
- Wellness Programs/Patient Engagement
The macro goal of this program is to improve patient outcomes with an integrated approach involving a 360° view of the patient. This full view into the world of the patient allows for risk stratification by cohort group and then predictive models can be utilized to classify patients by their levels of health risks. While this may sound highly futuristic today, there are tangible, actionable steps that can implemented now to begin down this path. As with any major organizational program involving significant change a phased-in deployment approach is considered a best practice.
Here are the four tangible areas to begin focusing on now:
- Follow the data, not your intuition. Big data is a key driver here as many healthcare data elements (+80%) are unstructured in nature. An agnostic view into aggregating these disparate data sets will insure interoperability across this entire data spectrum.
- Predictive analytics are needed to measure all the health/financial risks associated with the population group in areas such as readmission propensities etc. Risk scores are needed to quantify these risks levels by probabilities of such outcomes.
- Embedded analytics in the clinical workflows is a must to insure the right actions are taken at the right time by the right people in the patient care pathway. As an example in a pre-surgical setting a patient could have a high risk score for sepsis derived from real-time clinical data (lab results, prior case history etc.) and proactive preventive measures can be taken pre/post surgery to reduce the risk of sepsis.
- Data governance- “you get what you measure” is a time-tested adage. A visible data governance structure is a key driver for gaining executive sponsorship and support for a PH program. Data dashboards for all modalities of your data parameters are needed at all of the clinical touchpoints to insure an integrated coordination of care providers and to enable this 360° view of the patient population.
Connect with us to learn more about how our Population Health Assessment solution can help your healthcare organization get ready for this new emerging wave in healthcare management!

CMS Value-Based Payments Models
Financial risk on reimbursements is rapidly shifting away from the Payers to the Providers. It is widely known that value-based care is gaining acceptance in the healthcare industry, and is here to stay. CMS has a stated goal of moving 50% of their FFS payments into an alternate value-based payment model by 2018. And with most hospitals recognizing 35-45% of their revenues from CMS claims payments there are serious financial risks associated with these new initiatives that need to be effectively managed right now.
While it appears that the mandatory programs such as CJR and EPM are now out of favor with the new head of HHS; BPCI is still being offered in the voluntary participation mode along with the MSSP ACO program. The three primary tenets of both programs are care coordination, improving care quality, and better patient outcomes. And both programs have a goal of keeping care costs down below an established target/benchmark dollar amount. Many hospitals and physician groups are finding implementing a successful CMS value-based payment program to be problematic in many areas such as data analytics, care coordination, and real-time IT infrastructure. As an example, the MSSP ACO program only had 119 out of the 392 ACO’s generate earned shared savings monies in the 2015 performance year. And within BPCI only 25% of participants decide to move forward once the downside risk track begins in phase 2. So while these value-based programs have strong benefits for the Payer, healthcare providers continue to struggle with successfully implementing these program within their own organizations.
iCube’s current DUA (data use agreement) with CMS enables us to maintain a full in-house CMS claims data warehouse with 100% of the claims for 2016. This includes all the LDS datasets required to better understand your historical episode costs to allow for comparative benchmarking vs. any of your peers, and assess any gaps you might have that could be a potential roadblock for implementing and operating a successful program. Within BPCI target pricing is derived with 3 years of historical awardee claims data costs. And our predictive analytics platform called PQuintile PAC™ was built from scratch specifically for this CMS value-based payments program with major collaboration from various clinical and non-clinical experts to create a unique, one of a kind solution from our first module PQ Predict™ to PQ Act™ thru PQ Care™. With our full spectrum of data, services, and software tools our comprehensive solution we can help put you on the best path for your future success in these CMS programs.
Unlike other healthcare analytics firms, iCube’s PQuintile Risk Analytics Practice offers flexible service options to our healthcare clients from a full outsourcing of all your data analytics’ needs through doing one-off data analytics projects when the need arises. These options allow you to focus on your core capabilities of clinical and operation excellence while iCube does the data mining/heavy lifting for you. Or iCube can work in any other manner you’d like to enable your hospital to succeed in these CMS value-based payment models.
Is your healthcare organization ready to explore the world of value-based payments? If so let us do an initial CMS claims data assessment for you now to determine your best path forward.

Maximizer Hospital Profiles and Performance Metrics:
Our Maximizer hospital analytics platform contains a robust data set of 3000+ acute care hospitals in the USA. Comparative research work within geographic areas allows for a MSA peer group comparison or head to head with a particular hospital that is of interest.
1. Profile information such as number of inpatient days, average LOS, number of surgeries etc.:
- The most accurate and updated data on more than 3000+ ACH hospitals.
- Integrated affiliation data, which maps relationships among hospitals, IDNs, physicians, and other healthcare providers
- Detailed financial data and quality metrics, covering all CMS related payer initiatives
- Daily feed of RFPs across the various procurement categories within the hospital including technology, consulting, and major equipment purchase categories
- Robust analytics, including claims analytics and population health analytics that show where patients seek care across the entire care continuum
2. ACO/BPCI Data:
iCube’s database features the most up-to-date and in-depth data on over 800 Accountable Care Organizations (ACOs) and 200 Health Information Exchanges (HIEs), as well as Clinically Integrated Networks (CINs). This list of accountable care organizations and related organizations includes:
- Detailed ACO profiles including start date, patient population, number of physicians, and Medicare Shared Saving Program data
- Organization members including hospitals, payers, physician groups, and other healthcare providers
- Technology implementations
- Quality metrics
- Daily news and intelligence specific to these provider types
3. CMS Claims Data
- Maximizer is also powered by a 100% sample of the CMS inpatient claims data
- Claims data is down to the beneficiary level (without any PID level data)
- Claims data is curated at the hierarchy level starting with MS-DRG Code
- Enables medical procedure level analysis to identify hospitals with high volume of your targeted product areas
- LOS, readmissions, PAC discharge utilization by facility type metrics are also included


The PQ Predict tool helps in predicting the outcomes for individual patients and hospitals, clinical benchmarking in terms of KPIs, clinical decision support etc.; by analyzing information from historical and current data. The various data sources for this historical and current data include hospitals, Electronic health records, Clinical data (blood work etc.), Non clinical data etc.
- Hospital Performance Measurements and Prediction
- Enhanced Clinical Decision Support
- Financial and clinical Continuum-of-care Benchmarking
- Insights and Knowledge Management (Historical, Clinical & Non-Clinical)
- Growth Rate Simulation (Historic/ Payment Models)
- Patient Population/ Demographic Analysis
- DRG/ PAC Analysis
- Readmission Penalty Analysis
- Clinical Pathway Analysis
- Financial Comparative Modelling (FFS vs. Bundled Payments)
- Financial Payment Reconciliation (NPRA)
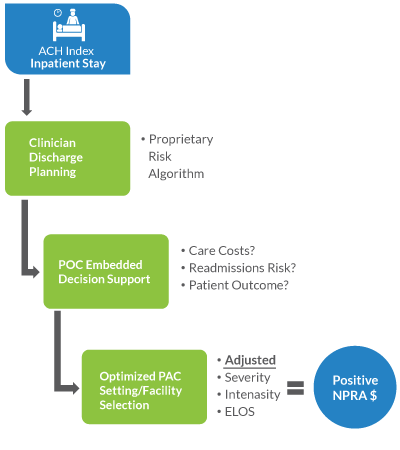
The PQ Act is the point of care solution for clinical and nonclinical staff of the ACH. It can be integrated with EHR systems to retrieve patient profile, get patient medical information, take patient surveys (like minicog…etc) and provide recommendations of discharge plan and PAC Distribution.
- Retrieve Patient Profile and Integrate with EMR
- Conduct Discharge Surveys (mini cog, etc.)
- Discharge Planning
- PAC Setting Recommendations
- Predict Optimal First PAC setting
- Predict PAC Length of Stay
- Predict Therapy Intensity
- Predict Expected Functional Improvement
- Predict Burden of Care following PAC discharge
- Predict Rate of Readmissions
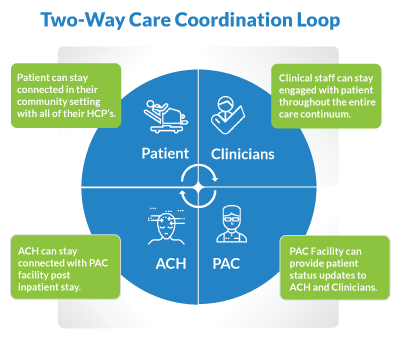
The PQ Collaborate tool helps in the care coordination and collaboration of ACH staff with ACH (client) partners. This enables the data capture of discharge handoff, patient monitoring, ability for PAC staff to input patient claims data, medical information, provide feedback etc.
- PAC Claims Management
- Patient Communications Management
- PAC Facility Performance Management
- Patient Monitoring and Tracking
- Patient Claims Info
- Multi-channel Communications Platform

Meet Dr.Oid
PQunitile™ PAC is powered by Dr.Oid ™, our cloud-based virtual physician that is derived from a series of Artificial Intelligent (AI) technologies and capable of providing predictive analytics, simulation and decision support. PQunitile™ PAC focuses on understanding patient outcome ‘impactability’ and optimizing patient care quality and cost of care during the post-acute care phase of the episode.
A major medical device company came to us with a challenging issue they were trying to solve for on a new product launch. The product had a strong clinical benefits profile with a unique MOA but they also wanted to create a unique economic story and use case around a new CMS initiative called Hospital Acquired Condition (HAC). ACA was becoming a reality and CMS was looking for ways to reduce the cost of healthcare for their inpatient beneficiaries.
The client felt if they had a strong economic case it would help build their distribution and sales volume much faster than launching with the clinical story alone. But they struggled coming up with a compelling value proposition and ROI for the product.
So we conducted customer research and came across an idea that synced up directly with the HAC initiative which was a hot button at the time. We developed a hospital analytics app that could quantify reductions in sepsis cases and the app could be used by the sales force at the individual hospital level to produce economic benefits metrics and ROI measures in real time right on their iPads.
With the new app the reps could prove out for the hospital procurement people how much money would be saved by using their product by reducing ICU LOS days and reducing mortality rates. Based on the average hospital volume the annual savings were approx. $500K with an ROI of almost 10 to 1.
The client deemed the solution to be a major component in making the new product launch highly successful.


